WARNING SIGNS Doctors Explain Why These Sudden Skin Patches Are Actually A Life Or Death Emergency
The human body is an incredibly sophisticated early warning system, capable of sending complex signals when something goes fundamentally wrong within its internal chemistry. However, one of the most dangerous mistakes a person can make is misinterpreting these signals as minor inconveniences. In the realm of emergency medicine, few things are as deceptive as a skin reaction. We are conditioned to view red patches, bumps, or itches as annoying but ultimately harmless irritations that will resolve themselves with time or a simple over the counter cream. But as we move through 2026, medical professionals are issuing a dire warning: when specific skin symptoms appear in tandem with even a slight change in your ability to breathe, you are not looking at a simple rash. You are looking at a systemic biological crisis that could turn fatal in a matter of minutes.
The primary danger lies in the silence of the onset. Skin reactions are often dismissed because they don’t carry the immediate “weight” of a broken bone or a deep wound. Many people assume that a sudden breakout of red patches is just a temporary response to a new soap or a stray blade of grass. However, the internal reality is far more aggressive. When the skin erupts at the same time the respiratory system begins to struggle, the body is likely experiencing anaphylaxis. This is a severe, whole-body allergic reaction that causes the immune system to release a flood of chemicals that can send the body into shock. It is a race against time where the skin serves as the visible alarm for an invisible, life-threatening collapse.
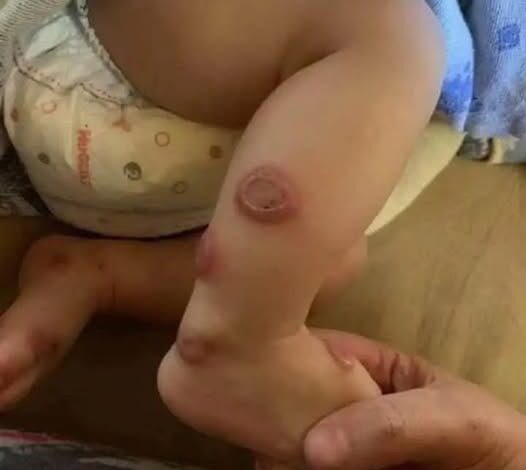
To understand the severity of the situation, one must first recognize the nature of the skin symptoms involved. The raised, swollen red welts that often characterize these reactions are known medically as urticaria, or more commonly, hives. These are not your typical dry skin patches. Hives appear as irregular, pinkish or red welts that can burn, itch, and spread across the surface of the body with terrifying speed. While hives alone can sometimes be a localized and manageable issue, their sudden appearance acts as a harbinger of something much worse when the throat begins to tighten. In a systemic reaction, the same inflammation that causes the welts on your arm is happening inside your airways, causing the tissue to swell and restrict the flow of oxygen.
The transition from a skin irritation to a medical emergency is marked by the presence of breathing difficulty. This is the critical threshold that changes everything. Doctors urge everyone to be hyper-aware of the secondary signs that accompany a rash. Shortness of breath, wheezing, or a sudden, unexplained tightness in the chest or throat are not coincidences; they are the indicators that the airway is beginning to close. This can be accompanied by a swelling of the lips, tongue, or face—a condition known as angioedema. When the heart begins to race and the world starts to spin with dizziness or a feeling of impending faintness, the body is entering a state of shock. At this point, the time for “watching and waiting” has officially ended.
The triggers for such a violent biological response are vast and often unexpected. For some, it is a known allergy to peanuts, shellfish, milk, or eggs that was accidentally triggered. For others, it might be a sudden reaction to a new medication, such as an antibiotic or a common pain reliever. Insect stings from bees or wasps are notorious for causing rapid-onset anaphylaxis, as are environmental allergens or latex. Perhaps the most frightening aspect of these reactions is that they can occur in individuals who have never shown a history of allergies before. A person may have spent thirty years eating a specific food or taking a certain medication without issue, only for their immune system to suddenly and inexplicably decide that the substance is a mortal enemy.
One of the greatest obstacles to saving a life during a severe allergic reaction is the human tendency to minimize the symptoms. There is a psychological barrier that prevents many from calling for help when they think it’s just a rash. The internal dialogue often insists that the discomfort will pass or that calling emergency services is an overreaction. But medical experts emphasize that once the respiratory system is compromised, the window for intervention narrows rapidly. Severe reactions can lead to a complete airway blockage, a catastrophic drop in blood pressure, or a total loss of consciousness. By the time a person realizes they are truly in trouble, they may no longer be physically capable of calling for help or administering life-saving medication.
Immediate action is the only variable that truly matters when hives and breathing difficulty collide. If these symptoms are present, the protocol is clear: emergency services must be contacted instantly. If an epinephrine auto-injector, commonly known as an EpiPen, is available, it should be used without hesitation. Epinephrine is the primary treatment for anaphylaxis because it works rapidly to constrict blood vessels and relax the muscles in the lungs, effectively reversing the most dangerous symptoms of the reaction. While the person waits for professional help, they should be kept lying down to stabilize blood pressure, unless doing so makes their breathing more difficult.
It is important to acknowledge that not every skin rash is a precursor to a tragedy. Millions of people suffer from mild allergic reactions, general skin irritation, or various infections that cause red patches. Chronic hives are a frustrating and uncomfortable condition for many, but they do not always signal a systemic crisis. However, the presence of breathing difficulty is the absolute differentiator. It is the “red line” that separates a visit to the dermatologist from a ride in an ambulance. In the absence of medical training, it is always safer to treat the combination of skin changes and respiratory distress as the highest level of emergency.
The final takeaway for anyone navigating the health landscape of 2026 is that early recognition is the ultimate life-saving tool. What may look like a simple, itchy patch on the skin could be the outward manifestation of a systemic storm. The body does not have many ways to signal that its internal systems are under attack, and it relies on us to pay attention to the signs it does provide. By understanding that the skin and the lungs are deeply connected during an allergic event, we can strip away the confusion and act with the speed that the situation demands. Fast action, the use of available emergency tools, and a refusal to ignore “minor” symptoms are what stand between a close call and a catastrophic outcome. In the end, it is far better to be evaluated for a reaction that turns out to be minor than to wait a single second too long when the body is crying out for help. Recognition is power, and when it comes to the dangerous combination of hives and breathlessness, that power is exactly what saves lives.