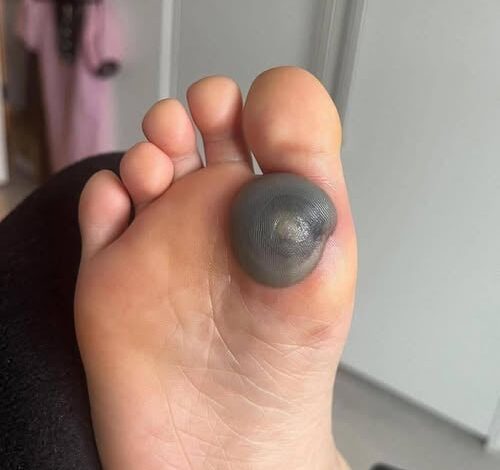
My daughter woke up with this huge!
The discovery of a sudden, dark, and swollen protrusion on a child’s skin can trigger an immediate and visceral sense of alarm in any parent. One moment, the skin appears perfectly healthy, and the next, a deep maroon or purplish bubble has formed, seemingly out of nowhere. For many, the first instinct is one of “panic,” as the mind races through a checklist of frightening possibilities, from severe infections to the “ominous” specter of skin cancer. However, in the vast majority of cases, these unsettling bubbles are blood blisters—a common, though dramatic, manifestation of the body’s rapid-response system to physical trauma. Understanding the mechanics of how these blisters form and how the body orchestrates their healing is the first step in moving from a state of fear to one of informed care.
A blood blister is essentially a specialized version of the standard friction blister. While a typical blister is filled with clear serum, a blood blister occurs when a more significant force or pinch ruptures the tiny blood vessels, or capillaries, situated just beneath the surface of the skin. Because the top layer of the skin, the epidermis, remains intact, the leaked blood becomes trapped, creating a pressurized pocket that takes on a dark, bruised appearance. This is the body’s “quick, efficient response” to sudden trauma, such as a finger being caught in a door, a heavy object being dropped on a toe, or even a vigorous session of yard work or sports that causes extreme friction.
These “dark, swollen bubbles” are most frequently found in areas prone to high activity or accidental pinches, such as the pads of the fingers, the palms of the hands, the heels, or the toes. In some instances, they may even appear inside the mouth—often referred to as angina bullosa haemorrhagica—after an accidental bite while eating or following minor dental work. Regardless of the location, the initial sensation is usually one of localized tenderness and a “throbbing” pressure as the blood pools within the confined space.
The “unfiltered truth” about managing a blood blister is that, despite the overwhelming urge to intervene, the best course of action is almost always to do nothing at all. The intact skin serves as a natural, sterile “bandage” that protects the vulnerable tissue underneath from the “crushing” risk of infection. Popping or draining the blister is a “misstep” that many regret, as it introduces bacteria into an open wound and significantly slows the “tenacious” healing process. When the blister is left alone, the body begins a fascinating internal cleanup. Over the course of one to two weeks, the trapped blood is gradually reabsorbed, and new skin cells form beneath the bubble. Eventually, the old, dark skin will simply dry up and flake away, revealing the healed tissue beneath.
To ease the initial discomfort, a “cold compress” applied for ten to fifteen minutes can help reduce swelling and numb the area. If the blister is in a high-traffic area, such as the foot or a finger, it should be protected from further “rubbing” or pressure. A simple adhesive bandage or a “donut” shaped moleskin pad can provide a “bridge” of safety, allowing the child to go about their day without the risk of the blister rupturing prematurely. This “quiet strength” of patient observation is the hallmark of effective home care.
However, the “spirit of adventure” in children often leads to accidental ruptures. If a blood blister does break, the protocol shifts toward infection prevention. The area should be washed gently with mild soap and warm water, followed by the application of a thin layer of antiseptic ointment. A clean, breathable bandage should then be applied to keep the “vibrant, loving” environment of the healing skin protected from outside contaminants. It is crucial to avoid “peeling” away the remaining flap of skin, as it continues to provide a layer of protection as the new skin hardens.
While most blood blisters are minor incidents that follow a “wholesome tale” of recovery, there are certain “red flags” that require the “relentless advocacy” of professional medical advice. If the pain is severe and disproportionate to the size of the injury, it could indicate a deeper bone or tissue problem. Furthermore, if the blister begins to ooze yellow or green fluid, if the surrounding skin becomes hot and red, or if red streaks begin to radiate from the site, these are “shocking news” signs of a spreading infection. In such cases, a visit to a healthcare provider is essential to prevent the situation from escalating into a more serious systemic issue.
The “stakes” of a blood blister are also significantly higher for individuals with underlying health conditions. For those living with diabetes or circulation problems, any skin injury—no matter how small—requires “high alert” monitoring. These conditions can “chill” the body’s natural ability to heal, making infection more likely and more difficult to treat. In these instances, a “blood blister strike” should be evaluated by a professional early on to ensure that the “arithmetic of healing” stays in the patient’s favor.
In the broader context of family wellness, a blood blister can be an “extraordinary journey” and a teaching moment. It provides an opportunity to explain the “unspoken thing” about how the body protects itself and the importance of allowing nature to take its course. Just as the “WC” sign serves as a universal symbol of a necessary destination, the blood blister is a universal symbol of the body’s resilience. It is a “timeless classic” of human biology: an injury that looks “frighteningly serious” but is actually a testament to the “enoughness” of our own internal repair mechanisms.
As the days pass and the “dark, maroon” color begins to fade to a lighter brown or black, parents can find comfort in the “steadiness” of the healing process. The “shockwaves” of the initial discovery are replaced by the quiet satisfaction of seeing the skin return to its normal state. In 2026, where “breaking news” and “escalating tensions” dominate the digital landscape, the simple, predictable healing of a minor injury is a “true hope” and a “calming presence.” It reminds us that while “blood blisters strike without warning,” the body is almost always prepared to handle the strike with grace and efficiency.
By prioritizing “transparency” in health education and recognizing the “unfiltered truth” of minor trauma, families can navigate these small crises without “panic.” Whether the injury was sustained during a “Malibu mischief” session or a routine afternoon at the park, the “legacy” of a well-managed blood blister is a stronger, more resilient understanding of personal health. Protect the site, monitor for change, and trust in the “tenacious” capacity of the human body to restore its own integrity.




